The Rise of Heart Disease in Millennials — What’s Behind It?
Written By - Elena Grant
on April 27, 2026
There was a time when heart disease felt like a problem reserved for retirement-age men, waiting rooms with outdated magazines, and someone saying the phrase “back in my day” at least twice. Not anymore. Today, more millennials are walking around with a heart risk profile that looks older than their driver’s license suggests. That does not mean every 30-year-old has a “bad heart,” and it certainly does not mean panic is useful. But it does mean the modern lifestyle is quietly stacking the deck in the wrong direction. Rising obesity and diabetes rates in adults ages 20 to 44, persistent high blood pressure, chronic stress, poor sleep, sedentary time, and highly processed diets are pushing cardiovascular risk earlier into adulthood. The scary part is not always dramatic symptoms. The scary part is how normal it can all feel while damage builds quietly in the background. If you’ve ever said, “I’m too young to worry about cholesterol,” your arteries may respectfully disagree. The good news? Early risk is exactly where prevention works best. When you build the habits early with the help of the heart-healthy diets for the better cardiovascular health will significantly reduce the long-term risk.
The 25 Going on 45 Phenomenon
You know that friend who says they’re “running on caffeine, vibes, and four hours of sleep”? Funny line. Terrible cardiology plan. What makes Heart Disease in Millennials feel so different is that it often behaves like a form of accelerated cardiovascular aging. That is not an official diagnosis, but it is a useful way to understand what’s happening: your birthday might say 29, while your risk factors are behaving like they’re already middle-aged. Blood vessels respond to pressure, inflammation, glucose swings, tobacco exposure, sleep loss, and inactivity over time. When those inputs pile up early, the heart and arteries start aging biologically faster than your calendar age. The American Heart Association notes that many people already have major risk factors by age 18, including high blood pressure, obesity, high cholesterol, or type 2 diabetes. Meanwhile, NHLBI reports that from 2009 to 2020, obesity and diabetes rose among young adults even as cholesterol improved modestly. In plain English: you can look young, feel busy, and still be quietly rehearsing for a heart problem your future self-did not book. The real issue is not one bad week of takeout or one stress spiral before a deadline. It is the repetition. When stress becomes your personality, screens become your hobby, and sleep becomes optional, the heart pays the subscription fee.
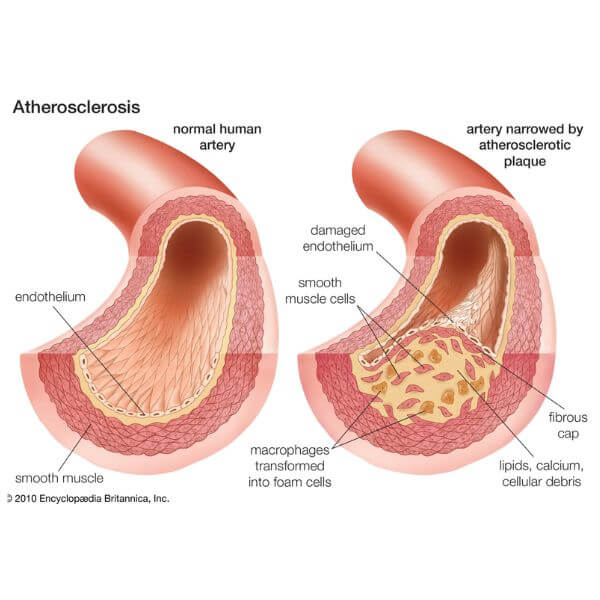
Inside Atherosclerosis — The Early Build-Up Nobody Feels
Here is the part nobody loves hearing: plaque buildup does not wait politely until you turn 60. Atherosclerosis begins early, often long before symptoms appear, and that is exactly why it is so easy to ignore. The process starts when fats, inflammatory cells, and other material begin collecting in the artery wall. Over time, those early fatty streaks can develop into firmer plaque that narrows blood flow or becomes unstable. You usually do not feel that happening. There is no dramatic pop-up notification from your chest saying, “Congrats, your arteries are now under construction.” A major review on younger-age atherosclerosis notes that the disease can begin in childhood and progress silently for years. One classic line of evidence found fatty streaks in the aortas of all studied individuals ages 2 to 39 who died from non-cardiac causes, and coronary fatty streaks in many children. More recent imaging also found evidence of coronary artery disease in one out of five people under 45 without known CAD. That matters because millennials often assume “no symptoms” means “no disease.” Unfortunately, the biology does not care about your assumptions. Plaque can be present, inflammation can be active, and your risk can be rising while you are still crushing your to-do list and pretending your energy drink is a personality trait. Diet has a very large role when it comes to the hidden triggers as the truth about the inflammation and everyday cooking oils is what many people overlook.
The Dopamine Lifestyle That’s Hurting Your Heart
Let’s be fair: your phone did not personally clog your arteries. But the dopamine-chasing lifestyle it encourages can absolutely create the conditions that make heart risk more likely. Constant alerts, endless scrolling, instant rewards, stress loops, late-night screen time, skipped workouts, stress eating, poor sleep, and sitting for hours at a stretch all nudge the body in the wrong direction. This is where brain chemistry and cardiovascular health start acting like very annoying roommates. Stress-related brain activity can increase heart rate, blood pressure, and inflammation, while anxiety and depression have been linked with higher cardiovascular risk through neural, autonomic, and inflammatory pathways. Mass General Brigham researchers reported that people with depression or anxiety had greater risk of major cardiovascular events, and those with both conditions fared worst. Add poor sleep to the mix and things get uglier: the American College of Cardiology highlighted research associating fewer than seven hours of sleep with a higher future risk of hypertension. Screen-heavy routines can also compound cardiometabolic risk, partly by pushing bedtime later and shortening sleep. So no, “dopamine” is not the villain in a cartoon-lab coat. The problem is the modern loop of over-stimulation, under-recovery, and chronic physiological strain. If your days are built on urgency and your nights are built on blue light, your heart may be working overtime for a lifestyle that still leaves you weirdly tired.
“I Feel Fine” — The Most Dangerous Sentence
If heart risk had better branding, more people would take it seriously. Instead, many cardiovascular problems are spectacularly quiet until they are not. High blood pressure is often called a silent threat for a reason. You can feel productive, social, gym-adjacent, and basically okay while your blood vessels are under constant strain. The same goes for high cholesterol and early plaque formation. Heart Disease in Millennials becomes dangerous when wellness is judged by vibes alone. “I feel fine” is comforting, but it is not a lab test, a blood pressure reading, or a lipid panel. The American Heart Association emphasizes that risk factors such as poor diet, inactivity, obesity, cholesterol problems, smoking, diabetes, sleep apnea, and stress can all operate without giving you a dramatic daily warning. Even when heart attack symptoms do appear, people often delay care because symptoms can begin slowly and feel mild at first. That is one reason prevention matters more than heroics. It is much easier to correct borderline cholesterol, early hypertension, or weight gain than it is to negotiate with a blocked artery later. Your body does not owe you obvious symptoms before asking for help. Sometimes the first “real sign” is the consequence. That is not fear-mongering. That is just how silent risk works. This is the reason why blood pressure should not be ignored even if you feel very normal.

Reverse Aging: Can You Actually Heal Your Heart?
Now for the part your nervous system deserves: this is not a doom story. In many cases, you can meaningfully improve cardiovascular health, reduce inflammation, improve blood pressure, lower cholesterol, improve insulin sensitivity, and slow or partly reverse the trajectory of damage with consistent changes. “Reverse aging” is a catchy phrase, but the real science is more practical and more encouraging: risk improves when your habits improve. Studies on intensive lifestyle change have shown that coronary disease burden can regress under the right conditions, and broad cardiovascular guidance remains clear on the fundamentals. A heart-smart pattern includes regular movement, not smoking, enough sleep, stress management, and a diet built around vegetables, fruits, whole grains, legumes, nuts, seeds, healthier fats, and lean proteins. Oily fish, fiber-rich foods, reduced sodium, and lower intake of ultra-processed foods all support the bigger picture. The goal is not perfection or becoming the kind of person who meal-preps eight identical mason jars on Sunday and posts about them with suspicious enthusiasm. The goal is consistency. Walk more. Sleep longer. Cook more often. Lift something heavy twice a week. Learn your numbers. Calm your nervous system before it starts running your life. The American Heart Association recommends at least 150 minutes of moderate activity weekly plus strength training on two or more days. That is not punishment. That is repair work your future heart will absolutely notice.
When you adopt the consistent routines such as weight loss habits that support the long-term metabolic health will further help you to accelerate the improvements in the cardiovascular markers.
Future-Proof Your Heart (Before It Bills You Later)
This is the grown-up part, but stay with me because it might save you money, stress, and a very unpleasant surprise. If you are in your 20s or 30s, prevention should not feel dramatic. It should feel routine. That means checking blood pressure, getting a cholesterol panel, discussing family history, and asking whether you also need testing such as Lp(a), ApoB, blood sugar, or other risk markers based on your personal profile. The American Heart Association now emphasizes that every adult 19 and older should have a cholesterol blood test panel, and newer risk tools are designed to think beyond the next 10 years. That matters because millennials often have long exposure time ahead, which means “borderline” today can become expensive tomorrow. And yes, sometimes lifestyle is enough. Sometimes it is not. If your LDL is elevated, your blood pressure is drifting up, or you have a strong family history, preventive medication may be part of the smartest plan. That is not failure. That is strategy. This is where a brand like GenPharmaRx fits naturally into the conversation: not as a panic button, but as a practical step after proper screening and clinician guidance. In other words, do not wait until your heart sends an invoice. Get checked, get informed, and if treatment is appropriate, explore licensed pharmacy options and evidence-based long-term management before “later” turns into “why didn’t I do this sooner?”
Final Takeaway
The rise of Heart Disease in Millennials is not about one villain. It is the result of a thousand ordinary choices that look harmless because they are normal. Chronic stress. Short sleep. Screen-heavy routines. Processed food. Inactivity. Untreated blood pressure. Quietly high cholesterol. The real shift happens when you stop treating heart health like a future problem and start treating it like current maintenance. Your heart is not asking for a total personality transplant. It is asking for fewer excuses and better systems. The earlier you respond, the more reversible the story becomes. So yes, you can absolutely keep your sense of humor. Just maybe pair it with a blood pressure cuff, a lipid panel, and a bedtime.
FAQ: Heart Disease in Millennials
Can millennials really get heart disease this early?
Yes. Heart disease risk factors can begin surprisingly young and atherosclerosis can start developing long before symptoms appear. The rise in the issues such as blood pressure and obesity, heavy stress and sleep loss are pushing the cardiovascular risk early to the adulthood.
Why are the heart related diseases not noticed in millennials?
Because many of the biggest drivers — high blood pressure, high cholesterol, insulin resistance, and early plaque buildup — can be silent. You may feel normal while risk builds in the background.
Is stress really that bad for the heart?
Chronic stress can raise heart rate, blood pressure, and inflammation. Stress is also linked to the actions that make the heart risk go bad which include the poor sleep, being inactive and being unhealthy by improper eating and smoking.
Is there any direct connection to social media and heart disease?
There is not a direct connection however a screen heavy and reward driven lifestyle can contribute to the poor sleep. This in return promotes the sedentary time and high cardio metabolic risk.
What are the earliest warning signs to watch for?
Sometimes there are no obvious signs. But chest discomfort, unusual fatigue, shortness of breath, dizziness, or high blood pressure readings should never be brushed off. If you suspect heart attack symptoms, seek emergency care immediately.
Can you reverse heart damage naturally?
You can often improve risk factors dramatically through lifestyle changes, and some studies suggest coronary disease can regress with intensive changes. But the degree of improvement depends on how early you act and your overall risk profile.
What diet can we intake for the millennial heart health?
A diet which includes the fruits, legumes and vegetables with nuts, seeds and leather protein. Healthy fats are strongly supported with lower sodium and few ultra-processed foods can also help.
How often should the young adults check cholesterol and blood pressure?
Adults of 19 and older than of that age should check the cholesterol and should visit the regular wellness which should include the blood pressure monitoring. The results may vary as per the family history and other risk factors.
If I exercise, can I ignore my cholesterol?
No. Exercise is powerful, but it does not cancel out genetics, high LDL, high blood pressure, diabetes, or a strong family history. Fitness helps, but it is not a hall pass from screening.
When should medication enter the conversation?
When your clinician sees persistent risk despite lifestyle changes, or when your numbers, family history, or overall risk profile justify earlier treatment. Preventive medication is a tool, not a defeat.
More Blogs